Mental Health Concerns
Psychologist vs Psychiatrist: Key Differences in Training, Treatment, & Career Path Explained

.png)
Written by
Aarohi Parakh,
Psychologist and Content Writer

Reviewed by
Sanjana Sivaram,
Psychologist and Clinical Content Head

Introduction
Mental health awareness in India has grown rapidly over the last decade. Conversations about anxiety, depression, trauma, and burnout are no longer confined to academic circles or urban elites. Yet one confusion remains extremely common. People still ask, “Should I see a psychiatrist or a psychologist?”
Both are mental health professionals. Both are trained to improve emotional wellbeing. Both work with individuals, couples, families, and sometimes organisations. However, their training, treatment approach, scope of practice, and role in managing severe mental health challenges differ significantly.
Choosing the right professional affects not just treatment outcomes but also time, cost, and expectations. Choosing a specialist who matches your needs helps ensure you receive the most appropriate and effective support from the start. This blog unpacks the differences in detail, from training pathways in India to prescription rights, therapeutic modalities, collaborative care, and career outlook.
Who Is a Psychiatrist? The Medical Route
The expression “psychiatry” is derived from the Greek term ‘psyche’, meaning “mind” or “soul,” and ‘iatreia’, meaning “healing.” Until the 18th century, mental illness was seen as demonic possession due to a lack of knowledge and superstition. However, it gradually came to be considered an ailment that requires treatment. Psychiatry is the branch of medicine that deals with the causes, diagnosis, preventive measures, and treatment of mental and behavioral disorders. Psychiatry is more inclined towards mental illnesses or disorders that can have a significant impact on patients′ quality of life, even life expectancy, and the patient/client may require a long-term or a life-long treatment.
A psychiatrist is a medical doctor who specialises in mental health. In India, this means completing an MBBS degree followed by a postgraduate qualification such as an MD (Doctor of Medicine) or DNB (Diplomate of National Board) in Psychiatry.
Core Role
Psychiatrists focus primarily on the biological and neurochemical factors influencing mental health. They assess how brain chemistry, genetics, hormonal imbalances, neurological conditions, and systemic illnesses contribute to psychological symptoms.
Their work sits at the intersection of psychiatry and general medicine. For example, thyroid dysfunction, vitamin deficiencies, epilepsy, head injuries, and substance use can all mimic or worsen psychiatric symptoms. A psychiatrist is trained to identify these overlaps.
Treatment Focus
The central area of expertise in psychiatry is psychopharmacology, which means medication management. Psychiatrists can prescribe antidepressants, mood stabilisers, antipsychotics, anxiolytics, selective serotonin reuptake inhibitors (SSRIs), and other psychiatric medications.
Treatments under a psychiatrist may include:
- Medication prescription and monitoring
- Adjustment of dosages
- Talk Therapy
- Laboratory investigations
- Managing side effects
- Medical interventions such as Electroconvulsive Therapy
- Transcranial Magnetic Stimulation in select cases
In India, Electroconvulsive Therapy is still used in severe and treatment-resistant depression, catatonia, and certain psychotic conditions. It is administered under anaesthesia in hospital settings and follows strict protocols.
When Psychiatry Becomes Essential
There are situations where consulting a psychiatrist is not optional but necessary. These include:
- Severe depression with suicidal thoughts
- Acute panic attacks with physical symptoms
- Substance withdrawal states
- Personality disorders, including borderline personality disorder (BPD), narcissistic personality disorder (NPD), obsessive-compulsive personality disorder (OCPD), and paranoid personality disorder (PPD)
In conditions such as schizophrenia or bipolar disorder, medication is often the foundation of treatment. Without stabilising neurochemical disturbances, psychotherapy alone may not be effective.
The Biological Lens
Psychiatrists are trained to think in terms of neurotransmitters, brain circuits, genetics, and systemic pathology.

This biological orientation does not mean psychiatrists ignore psychological factors. Many psychiatrists in India also offer brief counselling. However, their core competence remains in medical intervention.
Who Is a Psychologist? The Behavioural Route
The term 'psychology' derives from two Greek terms: 'psyche', which means mind, soul, or spirit, and 'logos', which denotes discourse or study. The combination of these words is 'Study of the mind'. Psychology first emerged as a discipline in its own right around 1879, when William Wundt opened the first psychology laboratory at the University of Leipzig in Germany. He and his colleagues were concerned with studying the mind via 'introspection', or observing their own thoughts and feelings as they occurred. These conscious mental processes were observed under carefully monitored circumstances, and the focus on measurement and control in these studies was what initially distinguished psychology from philosophy as a scientific field of study.
A psychologist is a trained mental health professional who specialises in human behaviour, cognition, emotions, and social interaction. A psychologist typically holds a Master’s or Doctoral degree (M.A./M.Sc. or Ph.D./Psy.D.). In India, a Clinical Psychologist is a professional who has completed an RCI-recognised MA in Clinical Psychology (formerly offered as the MPhil in Clinical Psychology, and planned to be phased out) and is registered with the Rehabilitation Council of India.
Only those registered under the Central Rehabilitation Register are legally permitted to use the title Clinical Psychologist in India. However, there is currently no licensing body for Counselling Psychologists in the country.
Core Role
Psychologists examine how thoughts, belief systems, trauma, developmental history, family dynamics, and cultural context influence mental health. Their framework integrates cognitive science, developmental psychology, behavioural learning theory, and trauma-informed practice.
Where psychiatrists are trained to evaluate neurochemical and biological factors, psychologists focus on psychological processes, environmental influences, and patterns of behaviour that maintain distress. Where psychiatrists ask, “What is happening biologically?”, psychologists often ask, “What meaning does this person attach to their experience?”
Treatment Focus
Psychologists specialise in evidence-based therapy modalities. Some of these include:
- Trauma-focused therapies
- Child and adolescent interventions
Clinical psychologists specifically are authorized to conduct psychological testing. This may include intelligence testing, personality assessment, neuropsychological screening, and diagnostic clarification for conditions such as ADHD, autism spectrum disorder, or learning disorders.
The Skills-Based Approach
Unlike medication, psychotherapy builds internal coping mechanisms. A psychologist helps clients:
- Identify cognitive distortions
- Regulate emotions
- Develop distress tolerance
- Process trauma
- Improve communication
- Modify maladaptive behaviours
- Strengthen self-awareness
For example, when someone struggles with anxiety, therapy helps them gradually face situations they’ve been avoiding and learn how to manage anxious thoughts more calmly.
When someone has experienced trauma, therapy provides a safe space to process what happened and teaches techniques to feel steady and present during emotional triggers.
In cases of relationship conflict, therapy focuses on improving communication, expressing needs clearly, and setting healthy limits.
Where Psychologists Are Often the First Choice
If you are navigating life transitions, academic stress, relationship breakdown, workplace burnout, or grief, a psychologist may be the most appropriate starting point.
In cases of mild to moderate depression or anxiety, psychotherapy alone can sometimes be sufficient. Research shows that Cognitive Behaviour Therapy is as effective as medication in many such cases.
Psychologists also play a crucial role in child guidance clinics, rehabilitation centres, schools, and corporate consulting settings.
Training and Education in India
Understanding training and education requirements helps clarify authority, scope of practice, and legal eligibility.
Psychiatry Timeline in India
- Undergraduate MBBS degree, five and a half years including compulsory internship
- Preparation and entrance examination for postgraduate specialisation
- MD Psychiatry or DNB Psychiatry, three years
- Optional senior residency or fellowship training, typically one to three years
From entry into medical school to independent specialist practice, the pathway usually spans 10 to 12 years, depending on fellowship and residency duration.
This training includes extensive exposure to general medicine, neurology, pharmacology, emergency psychiatry, and inpatient care.
Psychiatrists are registered medical doctors under the National Medical Commission and have full prescription rights, including the authority to manage complex medical and psychiatric comorbidities.
Psychology Timeline in India
- Undergraduate degree in Psychology, three or four years depending on programme structure
- Master’s degree in Psychology, typically two years (Counselling Psychologists)
- RCI recognised MA in Clinical Psychology, two years (Clinical Psychologists)
- Optional doctoral training such as PsyD or PhD for advanced clinical, academic, or supervisory roles
From entry into undergraduate education to independent licensed practice, the pathway typically spans 7 to 9 years, depending on academic progression and specialisation choices.
The MA in Clinical Psychology, which replaces the earlier MPhil route, includes intensive supervised clinical training in assessment, diagnosis, psychotherapy, and rehabilitation settings.
Upon completion, professionals must register with the Rehabilitation Council of India under the Central Rehabilitation Register to legally practice as Clinical Psychologists in India. Without RCI registration, one cannot use the protected title Clinical Psychologist.
International Comparison
In countries like the United Kingdom, psychologists complete doctoral-level training, such as a Doctorate in Clinical Psychology. Psychiatrists complete medical school followed by speciality training.
Although the pathways differ globally, the central distinction remains consistent. Psychiatrists are medical doctors. Psychologists are behavioural science experts.
Prescription Rights and Legal Scope
One of the clearest distinctions lies in prescription rights.
Psychiatrists in India can prescribe medication because they hold a medical degree. Psychologists cannot prescribe medication.
This does not imply one profession is superior to the other. It reflects different training models. Medication requires specialised medical knowledge. A psychiatrist must understand how a drug is absorbed and processed in the body, how it interacts with other medicines, when it should not be given, and how to handle any serious side effects safely. If a client in therapy requires medication, a psychologist will typically refer them to a psychiatrist while continuing psychotherapy.
Psychologist vs. Psychiatrist Comparison Table
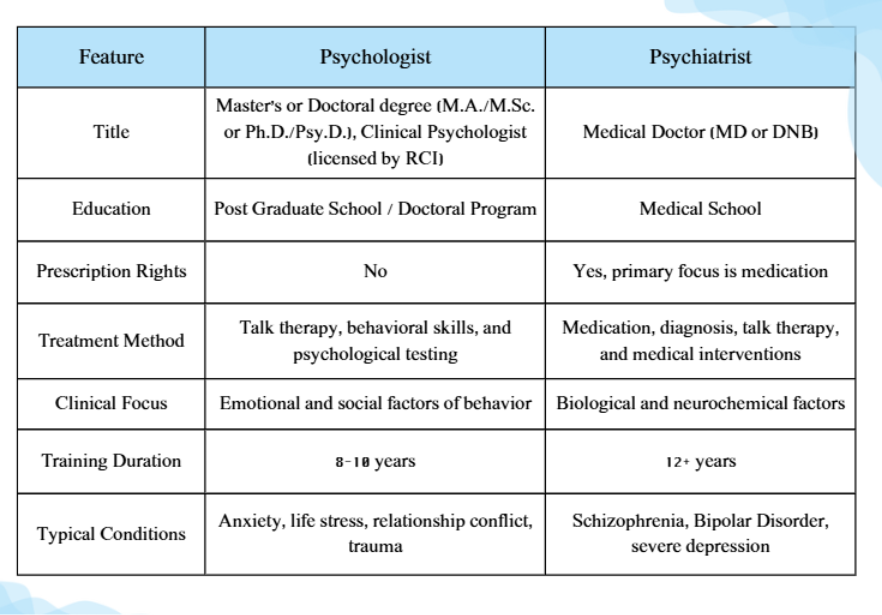
To make the distinctions clearer at a glance, here is a structured comparison of a psychologist and a psychiatrist across training, treatment approach, and scope of practice.
Severe Mental Illness and Complex Presentations
When dealing with severe mental illness such as schizophrenia, bipolar disorder, severe major depressive disorder with suicidality, or acute psychosis, psychiatric intervention is usually primary.
Medication stabilises acute symptoms. Once stabilised, psychological therapy becomes crucial for relapse prevention, functional recovery, and quality of life improvement.
In schizophrenia, antipsychotic medication reduces hallucinations and delusions. However, therapy helps improve social skills, insight, medication adherence, and vocational functioning.
In bipolar disorder, mood stabilisers manage manic and depressive episodes. Psychotherapy supports routine stabilisation, stress management, and family education.
Therefore, treatment is rarely either medication or therapy. It is often both.
Life Transitions, Trauma, and Relationship Conflict
Many individuals seek help not because of severe psychiatric illness but because life feels overwhelming.
Common concerns in Indian settings include:
- Academic pressure
- Career confusion
- Family conflict
- Marital discord
- Post-breakup distress
- Social anxiety
- Workplace stress or burnout
- Identity exploration
In such cases, psychotherapy is often the first-line intervention.
Therapy provides a structured space for reflection. It examines belief systems shaped by family, culture, and societal expectations. In the Indian context, factors such as patriarchy, collectivism, intergenerational living, and stigma significantly influence mental health.
A psychologist is trained to work within these sociocultural frameworks.
The Mind Body Connection
The mind-body connection is particularly relevant in Indian settings where somatic symptoms are common.
Many patients present with headaches, gastric issues, fatigue, and body aches rather than describing sadness or anxiety. A psychiatrist may rule out medical causes and prescribe medication if required. A psychologist may work on stress reduction, relaxation training, and cognitive restructuring.
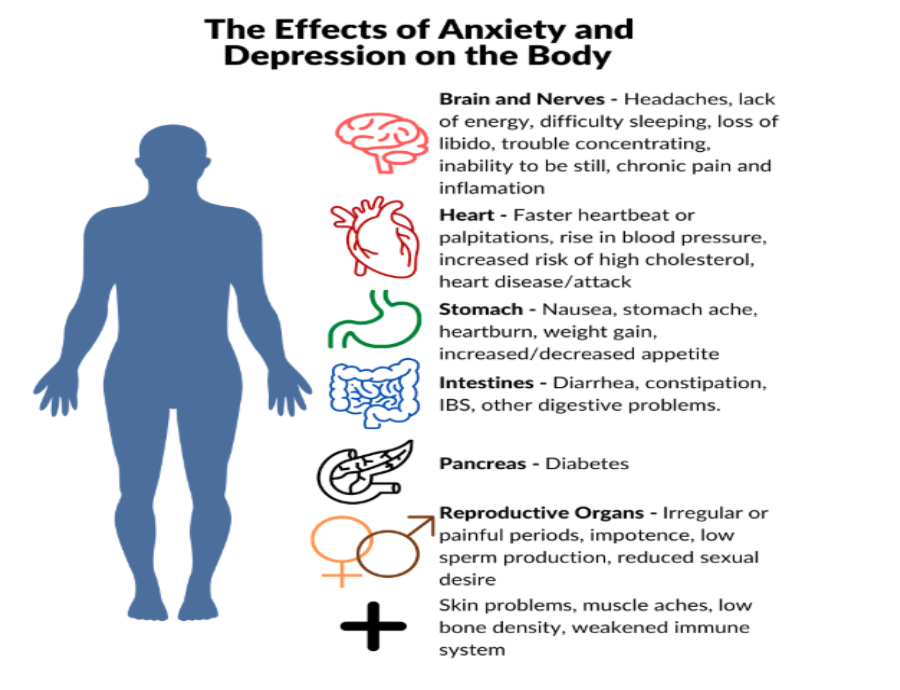
Both perspectives contribute to comprehensive care.
The Gold Standard of Care: Collaborative Approach
In ideal settings, psychiatrists and psychologists collaborate.
A typical collaborative model may look like this:
- Psychiatrist conducts medical evaluation and prescribes medication if needed
- Psychologist provides weekly psychotherapy
- Both professionals communicate regarding progress
- Medication adjustments are made alongside therapy insights
This integrated model is considered the gold standard of care, especially for moderate-to-severe conditions.
Unfortunately, in many parts of India, collaborative practice is still limited due to infrastructure and cost barriers. However, metropolitan centres are increasingly working towards adopting multidisciplinary frameworks.
Cost Considerations in India
Cost influences decision-making significantly.
Psychiatric consultations in urban India may range from moderate to high depending on the doctor’s experience. Medication adds recurring monthly costs.
Psychotherapy sessions are usually charged per session and require consistent attendance, often weekly. Over months, cumulative costs may become substantial. Nowadays, some psychologists also offer sliding scale charges for those who cannot afford the full price. Alternatively, there are also NGOs where affiliated psychologists offer session without payment/on pro-bono basis.
However, viewing therapy as skill-building rather than indefinite treatment helps contextualise the investment. Many clients attend therapy for a defined duration focused on measurable goals.
Career Outlook and Salaries in India
From a career perspective, psychiatry generally commands higher average earnings due to medical training and hospital affiliations. Private practice psychiatrists in metropolitan cities can earn substantially more than in salaried positions.
Clinical psychologists also earn competitively, especially in private practice, corporate consulting, rehabilitation centres, and academic institutions. Counselling psychologists, whether in independent practice or in settings such as schools or organisations, can earn competitively. However, the income gap between psychiatry and psychology persists due to differences in prescribing rights and hospital privileges.
Both professions are in demand. With increasing mental health awareness, schools, corporates, NGOs, and hospitals are expanding psychological services.
How to Decide Whom to See
You may consider seeing a psychiatrist if:
- Your symptoms are severe or disabling
- You have suicidal thoughts
- You suspect severe mental health challenges/disorders impacting your daily functioning
- You require a medical evaluation
- You need medication management
You may consider seeing a psychologist if:
- You want structured talk therapy
- You are navigating life stress
- You wish to process trauma
- You need behavioural change strategies
- You prefer non-medication approaches initially
In many cases, starting with either professional may eventually lead to referral to the other. What matters most is seeking help early rather than delaying support due to a lack of clarity.
Consultation Toolkit: Questions to Ask Before Seeking Help
- "Do you believe my symptoms require medication, or can we start with therapy alone?"
- "What is your philosophy on the mind-body connection?"
- "Do you collaborate with other mental health professionals if a different approach is needed?"
- "What specific therapeutic modalities (CBT, psychodynamic, etc.) do you specialize in?"
Final Thoughts
The debate of psychiatrist versus psychologist often creates unnecessary hierarchy. In reality, both professions address different dimensions of mental health. One approaches concerns from a medical and neurochemical standpoint. The other works through behavioural, cognitive, and psychosocial frameworks.
Mental health is multidimensional. Biological factors, psychological processes, social context, workplace pressures, and cultural influences interact continuously. Effective care acknowledges this complexity rather than reducing it to medication alone or therapy alone.
From an Indian perspective, increasing access to credible professionals, reducing stigma, and strengthening collaborative care models remain far more urgent priorities than choosing sides. The real question is not which profession is superior. It is the form of support you need at this stage of your journey.
If you are struggling, the most important step is reaching out early. Whether you consult a psychiatrist or a psychologist, timely intervention can significantly improve quality of life, functioning, and long-term resilience. Mental health care is not about labels. It is about restoring stability, clarity, and meaningful engagement with life.
For working professionals and organisations in India, structured support systems can make access easier. The Employee Assistance Programme by 1to1help offers confidential one-to-one sessions with qualified psychologists and, when clinically indicated, referrals to a trusted network of psychiatrists for medication management. If you are unsure where to begin, an EAP platform can provide guided access to the right level of care without the confusion of navigating the system alone.
FAQs
Q1. Can a psychologist prescribe medication in India?
No. In India, only a psychiatrist can prescribe medication, as they are medical doctors registered with the National Medical Commission. Clinical psychologists are registered under the Rehabilitation Council of India and specialise in psychotherapy and psychological assessment, but they do not have prescription rights.
Q2. Should I see a psychiatrist or psychologist first for anxiety or depression?
For mild to moderate anxiety or depression, many individuals begin with a psychologist for evidence-based therapy such as Cognitive Behaviour Therapy. If symptoms are severe, persistent, or include suicidal thoughts, consulting a psychiatrist for medical evaluation may be necessary. In many cases, both professionals work together.
Q3. Is medication always required for mental health conditions?
Not always. Some conditions respond well to psychotherapy alone, especially when symptoms are situational or linked to life stressors. However, severe mental illnesses such as bipolar disorder, schizophrenia, or major depressive disorder with high-risk factors often require medication as part of treatment. The decision depends on symptom severity, duration, and functional impairment.
Q4. What is the difference in training between a psychiatrist and a clinical psychologist in India?
A psychiatrist completes MBBS followed by MD or DNB Psychiatry, which typically spans around 10 to 12 years including training. A clinical psychologist completes a Bachelor’s and Master’s degree in Psychology followed by an RCI recognised MA in Clinical Psychology, usually spanning 7 to 9 years in total. Psychiatrists are trained in medicine and pharmacology, while psychologists are trained in psychotherapy and psychological assessment.
Q5. Can a psychiatrist and a psychologist treat the same patient together?
Yes, and this is often considered the best practice. A psychiatrist may manage medication and medical aspects, while a psychologist provides structured psychotherapy. This collaborative approach is especially effective for moderate to severe conditions that involve both biological and psychological factors.
Recommended Readings
References
- American Psychiatric Association. (n.d.). Diagnostic and statistical manual of mental disorders (DSM). https://www.psychiatry.org/psychiatrists/practice/dsm
- American Psychiatric Association. (n.d.). What is a substance use disorder? https://www.psychiatry.org/patients-families/addiction-substance-use-disorders/what-is-a-substance-use-disorder
- American Psychiatric Association. (n.d.). What is ADHD? https://www.psychiatry.org/patients-families/adhd/what-is-adhd
- American Psychological Association. (n.d.). Trauma. https://www.apa.org/topics/trauma
- Britannica. (n.d.). Psychological testing: Primary characteristics of methods or instruments. https://www.britannica.com/science/psychological-testing/Primary-characteristics-of-methods-or-instruments
- Cleveland Clinic. (n.d.). Anxiety disorders. https://my.clevelandclinic.org/health/diseases/9536-anxiety-disorders
- Cleveland Clinic. (n.d.). Depression. https://my.clevelandclinic.org/health/diseases/9290-depression
- Cleveland Clinic. (n.d.). Neurotransmitters. https://my.clevelandclinic.org/health/articles/22513-neurotransmitters
- Cleveland Clinic. (n.d.). Insomnia. https://my.clevelandclinic.org/health/diseases/12119-insomnia
- Cleveland Clinic. (n.d.). Cognitive behavioral therapy (CBT). https://my.clevelandclinic.org/health/treatments/21208-cognitive-behavioral-therapy-cbt
- Cleveland Clinic. (n.d.). Dialectical behavior therapy (DBT). https://my.clevelandclinic.org/health/treatments/22838-dialectical-behavior-therapy-dbt
- Cleveland Clinic. (n.d.). Family therapy. https://my.clevelandclinic.org/health/treatments/24454-family-therapy
- Cleveland Clinic. (n.d.). Antidepressants (depression medication). https://my.clevelandclinic.org/health/treatments/9301-antidepressants-depression-medication
- Cleveland Clinic. (n.d.). Mood stabilizers. https://my.clevelandclinic.org/health/articles/mood-stabilizers
- Cleveland Clinic. (n.d.). Antipsychotic medications. https://my.clevelandclinic.org/health/treatments/24692-antipsychotic-medications
- Cleveland Clinic. (n.d.). Anxiolytics. https://my.clevelandclinic.org/health/treatments/24776-anxiolytics
- Government of the United Kingdom. (n.d.). Working definition of trauma-informed practice. https://www.gov.uk/government/publications/working-definition-of-trauma-informed-practice/working-definition-of-trauma-informed-practice
- Healthline. (n.d.). Behavioral therapy. https://www.healthline.com/health/behavioral-therapy
- HopeWay. (n.d.). Schizophrenia spectrum and other psychotic disorders. https://hopeway.org/diagnoses/schizophrenia-spectrum-other-psychotic-disorders
- Mayo Clinic. (n.d.). Bipolar disorder. https://www.mayoclinic.org/diseases-conditions/bipolar-disorder/symptoms-causes/syc-20355955
- Mayo Clinic. (n.d.). Obsessive-compulsive disorder (OCD). https://www.mayoclinic.org/diseases-conditions/obsessive-compulsive-disorder/symptoms-causes/syc-20354432
- Mayo Clinic. (n.d.). Panic attacks. https://www.mayoclinic.org/diseases-conditions/panic-attacks/symptoms-causes/syc-20376021
- Mayo Clinic. (n.d.). Psychotherapy. https://www.mayoclinic.org/tests-procedures/psychotherapy/about/pac-20384616
- Mayo Clinic. (n.d.). Electroconvulsive therapy (ECT). https://www.mayoclinic.org/tests-procedures/electroconvulsive-therapy/about/pac-20393894
- Mayo Clinic. (n.d.). Transcranial magnetic stimulation (TMS). https://www.mayoclinic.org/tests-procedures/transcranial-magnetic-stimulation/about/pac-20384625
- Mayo Clinic. (n.d.). Selective serotonin reuptake inhibitors (SSRIs). https://www.mayoclinic.org/diseases-conditions/depression/in-depth/ssris/art-20044825
- News Medical. (n.d.). What is psychopharmacology? https://www.news-medical.net/health/What-is-Psychopharmacology.aspx
- Positive Psychology. (n.d.). Cognitive distortions. https://positivepsychology.com/cognitive-distortions/
- Positive Psychology. (n.d.). Body-mind integration and attention training. https://positivepsychology.com/body-mind-integration-attention-training/
- Rehabilitation Council of India. (n.d.). Regular mode courses. https://rehabcouncil.nic.in/regular-mode/
- Simply Psychology. (n.d.). Developmental psychology. https://www.simplypsychology.org/developmental-psychology.html
- World Health Organization. (n.d.). International classification of diseases (ICD). https://www.who.int/standards/classifications/classification-of-diseases
- Women’s Mental Health. (n.d.). Postpartum psychiatric disorders. https://womensmentalhealth.org/specialty-clinics/postpartum-psychiatric-disorders-2/





.png)