Workplace Well-Being & Support
Why Mental Health in the Workplace Matters More Than Ever

.png)
Written by
Aarohi Parakh,
Psychologist and Content Writer

Reviewed by
Sanjana Sivaram,
Psychologist and Clinical Content Head

Introduction
There is a quiet cost that does not show up on most balance sheets. It does not appear in quarterly earnings calls, and it rarely makes it to board presentations. But it is there, every single day, in the form of employees who are physically present but mentally absent, talented people who resign not because of the salary but because of how the workplace made them feel, and managers who notice something is wrong but have no idea what to do about it.
The importance of mental health in the workplace is no longer a conversation that organisations can afford to have in abstract terms. The evidence is clear, the costs are measurable, and the solutions are available; thus, inaction cannot remain a defensible position.
This blog makes the case in full. For business leaders, it makes the financial and strategic argument. For HR professionals, it provides a practical framework for what to do and how to measure it. For employees, it provides language and context to understand what they are experiencing and what they are entitled to expect from their workplace.
The Business Case for Workplace Mental Health
Let's start with the number that tends to stop conversations: the WHO estimates that depression and anxiety cost the global economy USD 1 trillion annually in lost productivity. That is not a public health statistic. That is a productivity and competitiveness crisis playing out inside organisations that have not yet connected the dots between their employees' mental health and their own financial performance. The connection is direct and well-documented. Employees who are struggling mentally are less focused, less creative, and less capable of the kind of decision-making that organisations depend on. They make more errors, miss more deadlines, and are significantly more likely to leave. The impact is not confined to individual performance. It ripples through teams, affects customer relationships, and ultimately shapes whether an organisation can execute its strategy.
The Return on Investment (ROI) case is equally compelling. Research consistently shows that for every dollar invested in workplace mental health support, employers can expect a fourfold return through reduced absence, lower turnover, and improved productivity. That is a 4:1 return, which is a better investment case than most capital expenditure decisions that make it into a boardroom.
The presenteeism problem is where the real cost hides. Absenteeism, days missed due to illness, is visible and measurable. Presenteeism, employees who show up but are operating well below their capacity due to unaddressed mental health challenges, is far harder to see and significantly more expensive. Employees with untreated mental health conditions lose an estimated 5.5 hours of productive work per week. Across a workforce of 500 people, with even a conservative estimate of 10% experiencing significant mental health challenges at any time, that represents over 14,000 hours of lost productivity per year.

The talent acquisition and retention angle is the one that most organisations feel most immediately. In today's labour market, employees, particularly those under 35, consistently cite mental health support as a key factor in job choice and retention decisions. Companies with strong mental health programmes see measurably lower voluntary attrition rates. According to SHRM, the cost of replacing an experienced employee ranges from 50% to 200% of their annual salary, depending on seniority and area of specialisation. A mental health programme that retains even two or three key people per year pays for itself many times over.
ROI Comparison: Cost of Inaction vs. Investment in Mental Health Programmes
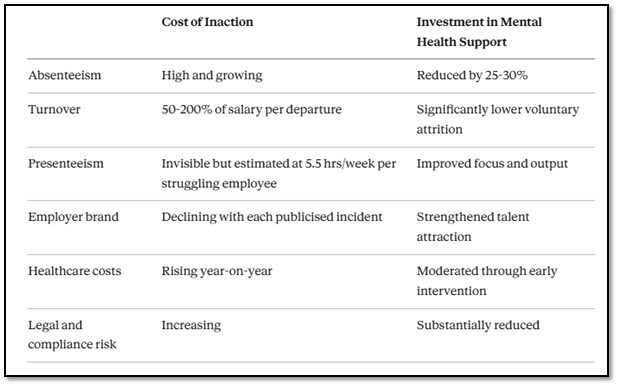
For a deeper dive into India-specific statistics on the cost of poor workplace mental health, see our companion piece: Mental Health at Workplace in India: A Complete Guide for Employers and Employees (2026)
Mental Health Challenges Affecting Today's Workforce
Before an organisation can address mental health effectively, it needs a clear picture of what it is actually dealing with. The most prevalent conditions in workplace settings are burnout, anxiety, depression, and the often invisible problem of presenteeism, where employees show up physically but are running well below capacity mentally. Alongside these clinical realities, there are workplace-specific drivers: excessive workloads, poor manager relationships, job insecurity, toxic culture, and, particularly in the Indian context, structural pressures around hustle culture, migration, and the weight of family expectations.
These challenges, their warning signs, their costs, and the specific way they manifest in Indian workplaces are covered in comprehensive detail in our dedicated guide. If you are building the internal case for mental health investment or trying to understand what your employees may be experiencing, that is the place to start.
What matters for the purposes of this article is the headline reality: globally, 1 in 5 working-age adults experience a mental health condition in any given year, and the majority do so without accessing professional support. In Indian workplaces specifically, approximately 42.5% of corporate employees are estimated to experience depression or anxiety, while the treatment gap sits between 70% and 92%. These are not edge cases happening in someone else's organisation. They are the baseline from which every mental health conversation at work needs to start.

How Mental Health Impacts Employee Engagement and Retention
Employee engagement research consistently identifies mental well-being as one of the strongest predictors of engagement scores. The Gallup research on employee engagement, which tracks over millions of employees globally, finds that psychologically safe workplaces see engagement scores that are multiple times higher than those where employees do not feel safe to speak up, make mistakes, or be honest about how they are doing.
The connection between mental health and engagement is not simply correlation. It is causal in both directions. Employees who feel mentally well are more engaged. Employees who are more engaged are less likely to experience burnout. The virtuous cycle runs in both directions, meaning that mental health investment is also an engagement investment.
Psychological safety is a term coined by Dr. Edmondson, a Harvard Business School Professor, and refers to a team climate in which members believe they will not be punished or humiliated for speaking up, asking questions, or making mistakes. It is the single best predictor of team performance identified by research, and it is deeply connected to mental health. A psychologically safe team is one in which mental health challenges can be acknowledged, where employees are not expected to act “fine” when they are struggling, and where managers are equipped to have honest conversations without triggering fear.
Building psychological safety requires specific, consistent leadership behaviours. It requires managers who model vulnerability, who respond to employee disclosures with empathy rather than judgement, who do not penalise mistakes but learn from them, and who create the regular, informal check-in moments that allow people to share how they are actually doing rather than only how their projects are tracking.
Retention data is unambiguous on this point. Organisations with strong mental health support programmes see lower voluntary attrition among employees who use them. Companies with EAPs and broader mental health initiatives report that employees who engage with mental health support are more likely to remain in employment, more likely to return to full productivity, and more likely to recommend the organisation as an employer.
Generational dynamics are accelerating this trend. Gen Z employees, who are entering the workforce with significantly higher mental health awareness than any preceding generation, consistently cite mental health benefits as a top priority in employer selection. For organisations competing for this talent, mental health support is no longer a differentiator. It is a basic expectation.

For more on how to build psychological safety and measure its impact on your workforce, see our guide: Mental Health at Workplace in India: A Complete Guide
Creating a Mentally Healthy Workplace Culture
Understanding the importance of mental health in the workplace is the starting point. The harder, more consequential work is building the conditions in which mental health can actually thrive. This is not accomplished through a single initiative or an annual awareness day. It is accomplished through sustained, consistent choices at every level of the organisation.
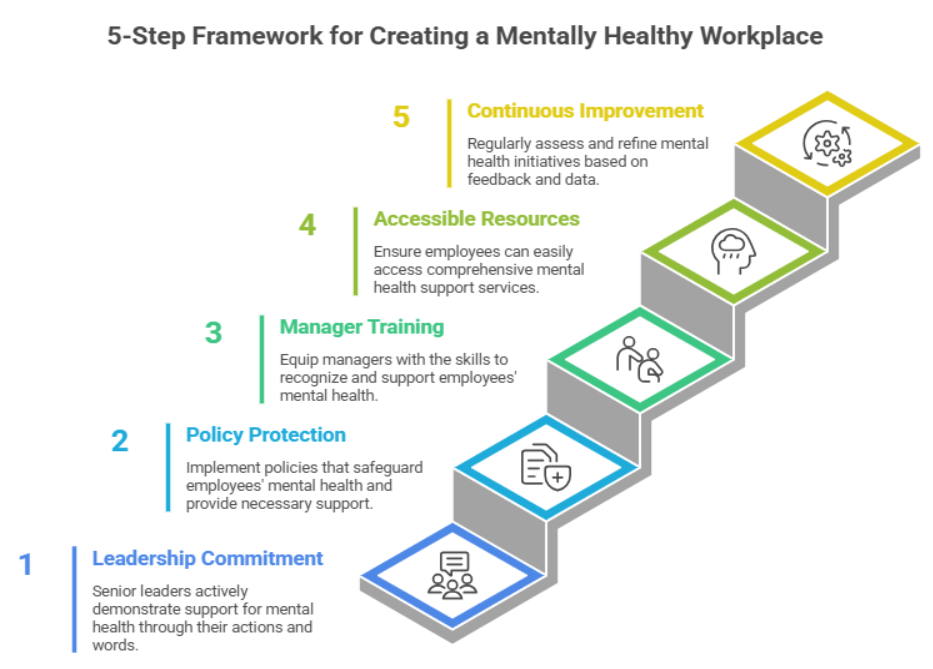
5-Step Framework for Creating a Mentally Healthy Workplace
Step 1: Leadership Commitment That Goes Beyond Words
Culture follows leadership. If senior leaders talk about mental health but work 70-hour weeks, send emails at midnight, and never show vulnerability or speak about their challenges, the cultural signal is clear: perform wellness, do not experience it. Genuine leadership commitment means visible behavioural change at the top, explicit endorsement of mental health as an organisational priority, and the willingness of senior leaders to model the vulnerability that creates permission for everyone else.
Step 2: Build Policy That Protects and Enables
Mental health-supportive policies include:
- confidentiality that assures employees their disclosures will not be used against them,
- anti-discrimination provisions that cover mental health conditions,
- flexible working arrangements that acknowledge the reality of how mental health is non-linear, and
- return-to-work programmes that ease reintegration after a mental health absence.
Policies also need to address performance management: employees experiencing mental health challenges or who have been diagnosed with mental health conditions may need adjusted timelines, modified workloads, or temporarily altered expectations. Building that flexibility into policy, rather than leaving it to individual manager discretion, creates consistency and reduces the risk of inadvertent discrimination.
Step 3: Invest in Manager Capability
Managers are the single most important lever in workplace mental health. Research consistently shows that the relationship with an immediate manager is one of the strongest predictors of an employee's mental health outcomes. A skilled, empathetic manager is one of the most effective mental health interventions available. An unskilled or unsupportive one is one of the most significant risk factors.
Manager training in mental health should cover: how to recognise the signs of mental health challenges in team members, how to have initial supportive conversations without overstepping clinical boundaries, how to connect employees to appropriate resources, how to adjust workloads and expectations appropriately, and how to manage their own mental health so they can lead with credibility. Programmes like 1to1help’s Emotional Care Champions (ECC) build this capacity internally by training employees to act as mental health allies.
Step 4: Provide Accessible, Comprehensive Resources
Knowing that support exists and knowing how to access it quickly and confidentially are different things. Resources need to be actively communicated, genuinely easy to access, and varied enough to serve employees with different preferences and levels of need.
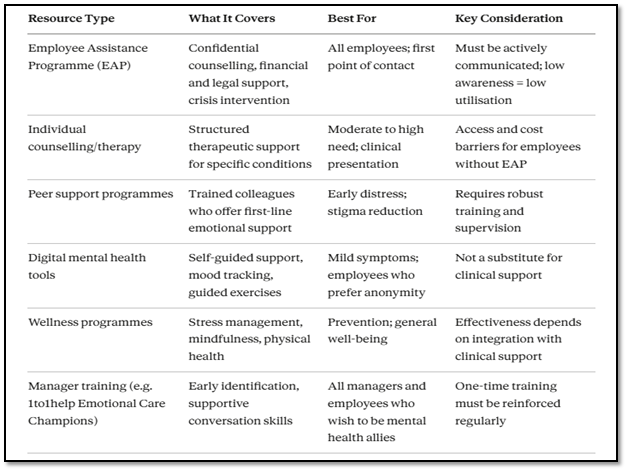
Step 5: Measure, Learn, and Improve
A mental health culture is not built once. It is built continuously, through the evidence you collect about what is working, what is not, and where the most significant needs are concentrated.

Mental Health Benefits for Different Workplace Sizes
One of the most persistent misconceptions about workplace mental health is that structured programmes are the domain of large enterprises with dedicated wellbeing teams and generous HR budgets. This is not accurate, and it is a misconception that costs smaller organisations considerably.
For small and medium-sized businesses, the most cost-effective starting points are often also the most impactful. Flexible working arrangements, which cost nothing to implement and significantly reduce stress-related absence, are available to any organisation. Manager training in mental health awareness can sometimes be a one-day investment that changes how an entire team operates. Anonymous pulse surveys, which can be run through free digital tools, provide the data needed to understand where attention is most needed. Many EAP providers offer scalable options for organisations with fewer than 100 employees, at costs that are significantly lower than the turnover costs they prevent.
Peer support programmes are particularly powerful in smaller organisations, where informal relationships are stronger, and the network of trusted colleagues is closer. A trained peer supporter in a team of 20 can reach employees who would never proactively seek formal support.
For larger organisations, the challenge is less about access to resources and more about consistency, measurement, and cultural change at scale. Enterprise-level mental health strategies need to address multi-location coordination, ensuring that the quality of mental health support does not vary significantly based on which office or region an employee works in. Data analytics become important at this scale: understanding which departments, which roles, and which demographic segments are experiencing the highest mental health risk allows for targeted rather than generic interventions.
Large organisations also have the opportunity and the responsibility to use their resources to influence the quality of mental health provision available to their employees. Selecting EAP providers that generate robust reporting data, offer multilingual and multichannel access, and can demonstrate outcome metrics gives HR teams the evidence they need to continuously improve their offerings.
Remote and hybrid workers present a specific challenge that deserves explicit attention regardless of organisation size. The isolation of remote work, the blurring of home and work boundaries, and the absence of informal social connections that office environments provide all create elevated mental health risk. Digital-first mental health support, proactive rather than reactive outreach from managers, and deliberate efforts to create connections within distributed teams are all necessary components of a mental health approach that works for the modern workforce.

Measuring Success: Mental Health Metrics and KPIs
An organisation that invests in mental health without measuring the outcomes is operating on faith rather than evidence. Measurement serves two purposes: it tells you whether your interventions are working, and it provides the data you need to justify continued investment to finance and leadership.
Key metrics to track:
- Absenteeism rate is the most straightforward starting point. Calculate it as total days absent due to illness divided by total available working days, expressed as a percentage. Track this monthly and segment by department to identify where absence rates are highest. A sustained reduction following mental health investment is one of the clearest indicators of programme effectiveness.

- Voluntary turnover rate among employees who have accessed mental health support versus those who have not is a comparison that consistently demonstrates programme value. If supported employees are leaving at a lower rate, the programme is generating measurable retention value.
- EAP utilisation rate tells you whether your support resources are actually being accessed. Industry benchmarks suggest healthy utilisation sits between 5% and 10% of eligible employees per year. Rates below 5% indicate communication, trust, or accessibility barriers that need attention.
- Employee Net Promoter Score (eNPS) and engagement surveys provide leading indicators of mental health culture. Questions about psychological safety, manager support, and workload manageability provide early warning signals before they manifest as absenteeism or attrition.
- Return-to-work rates following mental health-related absence measure how effectively your organisation supports employees through recovery and reintegration. Higher return-to-work rates indicate that the support provided during absence is effective and that the return process is managed sensitively.
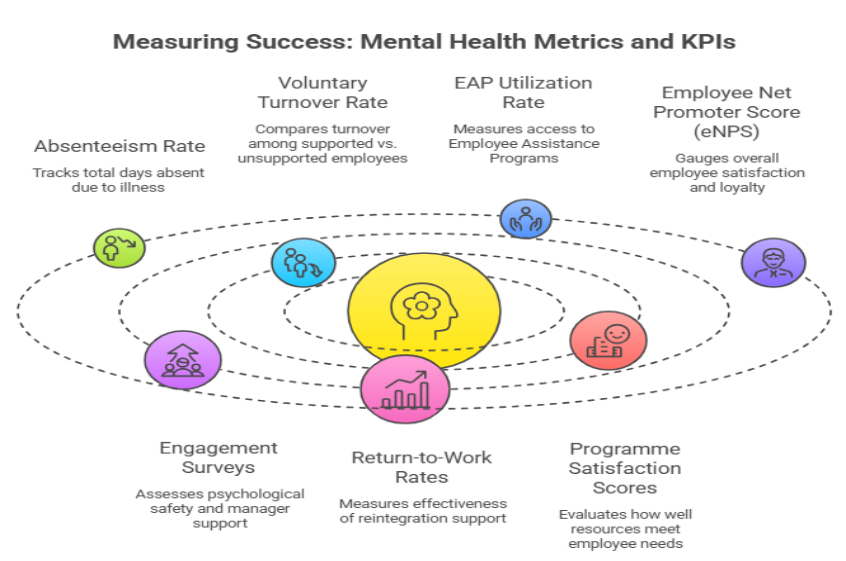
- Programme satisfaction scores from employees who use mental health resources tell you whether the resources are meeting their needs. A programme that receives consistently low satisfaction scores is not serving its purpose, regardless of how much it costs or how impressive it looks on paper.

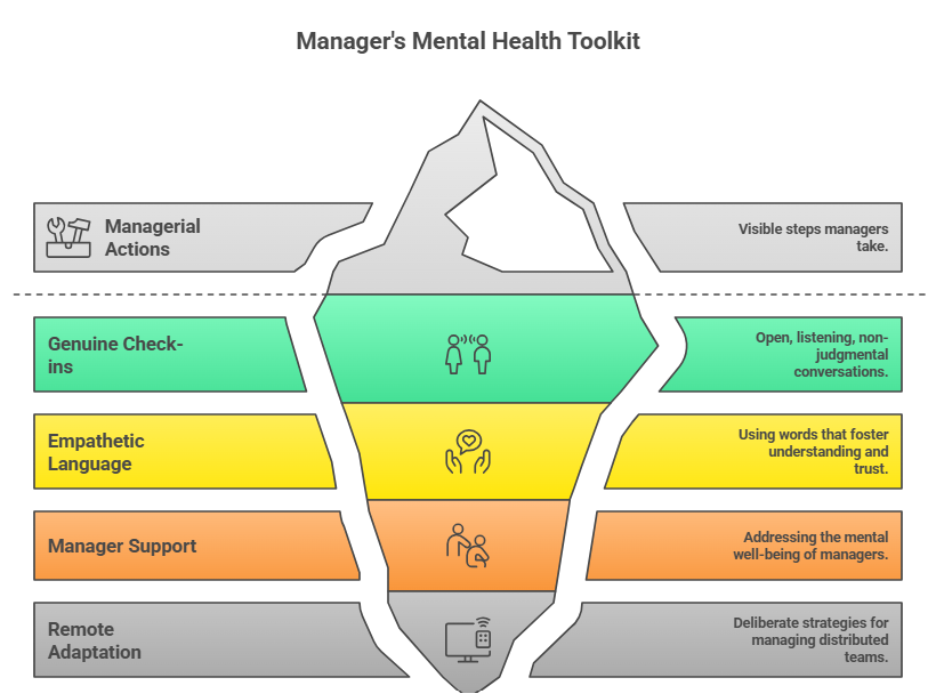
The Manager's Mental Health Toolkit: Unique Angles for Making This Real
Most guidance on workplace mental health addresses what organisations should do. Less attention is paid to the specific, practical tools that managers need to make it real in their teams day to day. Here is what that looks like in practice.
The check-in that actually checks in. Most one-to-ones are agenda-driven and output-focused. A genuine mental health check-in looks different: it starts with an open, specific question ("You've seemed quieter this week. How are things?"), it allows silence and does not rush to fill it, and it focuses on listening rather than solving. The goal is not to diagnose or to counsel. It is to signal that you notice and that you care.
Language matters more than most managers realise. The difference between "I've noticed your performance has slipped" and "I've noticed things feel different for you lately and I wanted to check in" is the difference between triggering defensiveness and opening a door for genuine conversation. Training managers in the specific language of mental health conversations is one of the highest-value investments an organisation can make.
Managers need support too. One of the most overlooked dimensions of workplace mental health is the mental health of managers themselves. Managers carry the stress of their roles while also being responsible for their teams' well-being. Organisations that invest only in employee-facing mental health support while ignoring manager mental health create a structural inconsistency: they ask people who are themselves unsupported to support others. Manager well-being needs to be explicitly included in any mental health strategy.
Remote and hybrid management requires specific adaptation. The informal check-ins that happen naturally in office environments, the five-minute conversation at the coffee machine, the ability to notice that someone looks tired or stressed, do not happen automatically in remote settings. Managers of distributed teams need to be more deliberate: scheduling brief, informal catch-ups that have no agenda, using video rather than chat for sensitive conversations, and actively working to maintain the social fabric of a team that does not share a physical space.
A Final Word: From Importance to Action
The importance of mental health in the workplace has never been more widely understood. The evidence base is solid, the business case is clear, and the tools to act are available and increasingly accessible.
What most organisations still need is not more information. It is the translation of what they know into what they do: consistent, specific, measurable action that reaches employees before distress becomes crisis and that treats mental health as a strategic organisational priority rather than an HR programme.
The organisations that will attract and retain the best talent, build the most resilient cultures, and perform most consistently over the next decade will be the ones that take that step.
Ready to Build a Mentally Healthier Workplace?
For organisations that are ready to move from good intentions to structured action, 1to1help's Employee Assistance Programme is India's most trusted EAP, with over 25 years of experience supporting employees across more than 700 organisations nationwide. From confidential counselling and crisis support to manager training and organisational well-being assessments, 1to1help offers a comprehensive, culturally sensitive, and multilingual solution tailored to the Indian workplace.
With data from over 100,000 counselling sessions annually and outcomes that include a 53% reduction in depression symptoms and a 48% reduction in anxiety within just a few sessions, 1to1help's programmes are evidence-based, scalable, and designed to meet your employees where they are, whether they are in a metro office, working remotely, or based in a Tier 2 city.
The strongest workplaces are built on psychological well-being, not just productivity.
FAQs
Q1. What is the importance of mental health in the workplace?
Mental health in the workplace affects every dimension of how an organisation performs. It shapes employee productivity, engagement, retention, and the quality of decisions people make. Organisations that support employee mental health see measurable improvements in attendance, output quality, and talent retention. They do not pay a consistent, compounding cost in absenteeism, turnover, and lost performance.
Q2. How does mental health affect workplace productivity?
Poor mental health reduces concentration, impairs decision-making, increases error rates, and drives presenteeism, where employees are physically present but mentally disengaged. Employees with unaddressed mental health conditions lose an estimated 5.5 hours of productive work per week. Across a workforce of any significant size, this represents a substantial and measurable productivity loss.
Q3. What are the signs of mental health issues at work?
Signs include withdrawal from team interactions, declining performance quality, increased absences, difficulty concentrating, irritability, apparent exhaustion, and expressions of feeling overwhelmed. None of these signs are individually diagnostic, but a pattern across two or more weeks is a prompt for a supportive check-in conversation.
Q4. How can employers support employee mental health?
Employers can support mental health through a combination of leadership culture (modelling openness and reducing stigma), policy (flexible working, confidentiality protections, reasonable adjustments), resources (EAPs, counselling access, digital tools), manager training, and consistent measurement. Effective mental health support is systematic rather than episodic.
Q5. What is an EAP and how does it help employees?
An Employee Assistance Programme is a confidential support service that gives employees access to counselling, legal advice, financial guidance, and crisis support, typically at no personal cost. EAPs are most effective when employees trust that their usage is genuinely confidential, when they are actively communicated rather than buried in a benefits document, and when they are part of a broader organisational commitment to mental health rather than the only provision available.
Q6. How do I talk to my manager about mental health at work?
Choose a private setting and a moment when neither of you is under immediate pressure. Frame the conversation around your work experience rather than a clinical label: "I've been finding it harder to focus lately and I wanted to talk about whether there's any flexibility available." You do not need to disclose a diagnosis to ask for support or adjustments. If your organisation has an EAP or HR helpline, these may be more comfortable entry points than a direct manager conversation.
Q7. What mental health resources should companies provide?
At minimum: a confidential EAP with counselling access, a clear policy on mental health absence and return to work, manager training in mental health awareness, and active, regular communication about what support is available. Better practice adds digital mental health tools, peer support programmes, regular pulse surveys, and explicit psychological safety initiatives. Best practice integrates all of these into a coherent, measured strategy with named ownership and regular leadership review.
References
- World Health Organization. (n.d.). Mental health in the workplace. https://www.who.int/teams/mental-health-and-substance-use/promotion-prevention/mental-health-in-the-workplace
- World Health Organization. (2019, May 28). Burn-out an occupational phenomenon: International classification of diseases. https://www.who.int/news/item/28-05-2019-burn-out-an-occupational-phenomenon-international-classification-of-diseases
- American Psychological Association. (n.d.). Psychological safety in the workplace. https://www.apa.org/topics/healthy-workplaces/psychological-safety
- BetterUp. (n.d.). Mental health in the workplace. https://www.betterup.com/blog/mental-health-in-the-workplace
- Harvard Business School. (n.d.). The $1 trillion link between mental health and economic productivity. https://www.library.hbs.edu/working-knowledge/the-usd1-trillion-link-between-mental-health-and-economic-productivity
- McKinsey & Company. (n.d.). Thriving workplaces: How employers can improve productivity and change lives. https://www.mckinsey.com/mhi/our-insights/thriving-workplaces-how-employers-can-improve-productivity-and-change-lives
- National Center for Biotechnology Information. (2024). Workplace mental health research study. https://pmc.ncbi.nlm.nih.gov/articles/PMC12375206/
- National Center for Biotechnology Information. (2022). Workplace mental health interventions review. https://pmc.ncbi.nlm.nih.gov/articles/PMC9663290/
- Investopedia. (n.d.). Return on investment (ROI). https://www.investopedia.com/terms/r/returnoninvestment.asp
- Investopedia. (n.d.). Presenteeism. https://www.investopedia.com/terms/p/presenteeism.asp
- AIHR. (n.d.). Absenteeism: Definition and impact. https://www.aihr.com/blog/absenteeism/
- AIHR. (n.d.). Voluntary turnover. https://www.aihr.com/blog/voluntary-turnover/
- AIHR. (n.d.). Employee Net Promoter Score (eNPS). https://www.aihr.com/blog/employee-net-promoter-score-enps/
- Gallup. (n.d.). Employee engagement and performance. https://www.gallup.com/workplace/285674/improve-employee-engagement-workplace.aspx
- Gallup. (n.d.). Q12 employee engagement survey. https://www.gallup.com/q12-employee-engagement-survey/
- Cleveland Clinic. (n.d.). Anxiety disorders. https://my.clevelandclinic.org/health/diseases/9536-anxiety-disorders
- Cleveland Clinic. (n.d.). Depression. https://my.clevelandclinic.org/health/diseases/9290-depression
- Government of India, Press Information Bureau. (n.d.). Mental health statistics in India. https://www.pib.gov.in/PressNoteDetails.aspx?NoteId=153261&ModuleId=3®=3&lang=1
- Anbessa, M. (n.d.). Impact of mental health on workplace productivity. LinkedIn. https://www.linkedin.com/pulse/impact-mental-health-workplace-productivity-anbessa-mundus-qcpdf/
- Society for Human Resource Management. (n.d.). The myth of replaceability. https://www.shrm.org/in/executive-network/insights/myth-replaceability-preparing-loss-key-employees
- Meditopia. (n.d.). EAP statistics and utilization rates. https://meditopia.com/en/forwork/articles/eap-statistics-and-utilization-rates
- Sonder. (n.d.). Average EAP utilisation rates. https://sonder.io/resources/blog/average-eap-utilisation-rates/
- Qualtrics. (n.d.). Employee engagement surveys. https://www.qualtrics.com/articles/employee-experience/employee-engagement-survey/
- Keka. (n.d.). How to conduct a pulse survey. https://www.keka.com/how-to-conduct-pulse-survey
- IE University. (n.d.). Decoding Gen Z: Why mental health matters at work. https://www.ie.edu/talent-careers/news-and-events/news/decoding-gen-z-why-mental-health-matters-work/
- Careerizma. (n.d.). Depression statistics in India. https://www.careerizma.com/blog/depression-india-statistics-causes-symptoms-treatment/
- ResearchGate. (n.d.). Psychological safety and employee engagement. https://www.researchgate.net/publication/399166630_Psychological_Safety_and_Its_Impact_on_Employee_Engagement_Implications_for_Management
- Nobl. (n.d.). Google’s high-performing teams. https://nobl.io/changemaker/google-high-performing-teams/





.png)