Mental Health Concerns
What is Behavioral Health? A Complete Guide for the Indian Workplace (2026)

.png)
Written by
Aarohi Parakh,
Psychologist and Content Writer

Reviewed by
Sanjana Sivaram,
Psychologist and Clinical Content Head

Introduction
Riya is a high-performing project manager at a Bengaluru IT firm. Her team consistently hits targets. Her annual appraisals are strong. She also drinks two large pegs of whisky every night to wind down, has not slept more than five hours in eight months, and has not disclosed either fact to anyone at work. Her manager thinks she is fine. Her HR team has no idea. Her Employee Assistance Programme (EAP), introduced last year with minimal communication, has never been accessed by anyone on her floor.
Riya's situation is not unusual. It is the norm across a significant portion of India's urban workforce. And it sits squarely within the scope of what health professionals and HR leaders mean when they talk about behavioral health. She is experiencing something that behavioral health is designed to address, where behaviour, physical health, and psychological safety are all interconnected and cannot be understood in isolation.
This guide explains what behavioral health means, why it matters in the Indian workplace, what services and legal frameworks exist, and how organisations can move from good intention to practical, measurable support for the people who work for them.

What is Behavioral Health?
Behavioral health is a broad term that describes the relationship between an individual's behaviours, habits, and their overall mental and physical wellbeing. It goes beyond mental illness alone to include how daily actions such as sleep patterns, diet, substance use, exercise, and stress responses interact with and shape a person's health.
More than 1 billion people are living with mental health disorders, according to new data released by the World Health Organization (WHO), with conditions such as anxiety and depression inflicting immense human and economic tolls. In India, the National Mental Health Survey places the number of people living with mental disorders at over 197 million.
The distinction between mental health and behavioral health is important for shaping effective workplace policies. Mental health refers primarily to a person's emotional and psychological state: how they think, feel, and relate to others. Behavioral health broadens this frame to include the behaviours that reinforce, undermine, or create those states. Alcohol use, sedentary habits, poor nutrition, disordered sleep, excessive screen time, and maladaptive coping patterns are behavioral health concerns that sit upstream of clinical diagnoses.
Behavioral Health vs Mental Health: A Direct Comparison
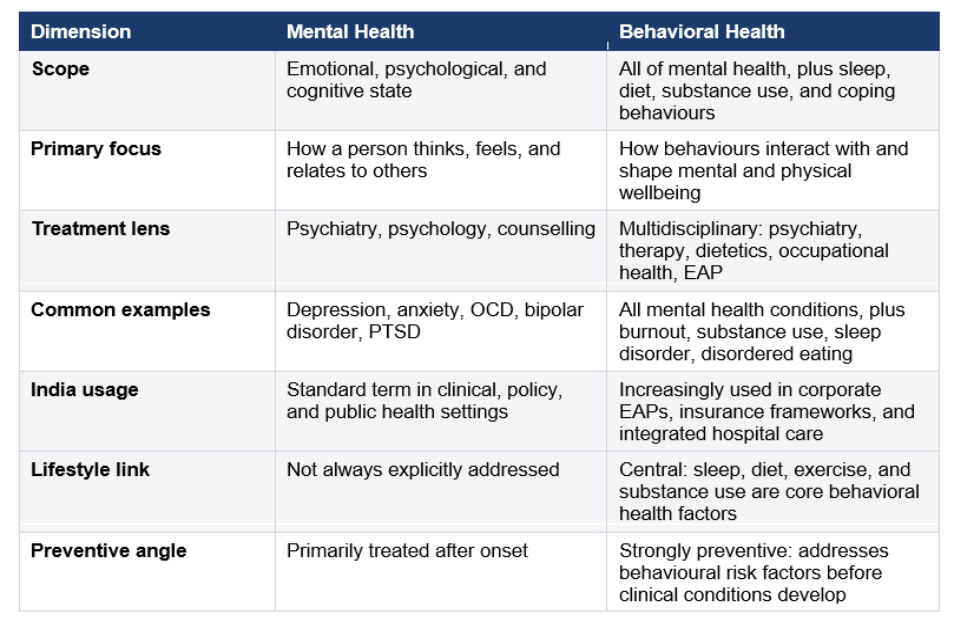
Behavioral Health Meaning in the Indian Context
Behavioral health meaning is still being established in Indian corporate and healthcare settings. The term is gaining traction within EAP frameworks, insurance policy language, and integrated hospital care, driven in part by global HR standards and in part by India's evolving legal landscape. The Mental Healthcare Act 2017 broadens the rights-based approach to mental and behavioral conditions, establishing clear protections around access to care and non-discrimination in employment. The International Classification of Diseases (ICD-11) and the Diagnostic and Statistical Manual of Mental Disorders (DSM-5-TR) remain underutilised in the workplace settings, creating an awareness gap that the behavioral health framework is well-positioned to address.
India Focus: In India, the word 'behavioral health' often generates confusion: HR teams ask whether it is the same as mental health, while clinicians use it inconsistently. The practical distinction that matters most for Indian workplaces is this: mental health is a destination, behavioral health is the map. A behavioral health approach asks not just 'is this employee depressed?' but 'what patterns are driving or preventing recovery?' That question changes both the conversation and the intervention.
Why Behavioral Health Matters in the Indian Workplace
The business and human case for taking behavioral health in the workplace seriously in India is not aspirational. It is evidence-based, quantified, and growing.

These numbers describe a workforce under significant, sustained pressure. Deloitte's 2022 Mental Health and Employers Report on India found that 80% of Indian employees reported mental health challenges affecting their work, yet organisational response remains fragmented. A 2024 EAP Industry Report by the Employee Assistance Professionals Association found that 78% of Indian employees who needed mental health support in the past year did not access their EAP. Of those, 61% cited concern about confidentiality, 48% cited inconvenience or access barriers, and 39% cited stigma. A 2023 NIMHANS study found that 67% of Indian employees believe seeking mental health support through employer-provided programs could affect their career prospects. Perception is reality when it drives behavior, and this perception drives non-utilization.
How Behavioral Health Affects Workplace Productivity in India
Poor workplace behavioral health creates four cascading organisational costs:
- Reduced productivity: impaired focus, slower decision-making, and lower creative output in employees managing unaddressed behavioral health conditions
- Absenteeism: days lost to episodes of acute mental and physical distress that could have been prevented with earlier intervention
- Presenteeism: the hidden cost of employees who are physically present but mentally disengaged; research suggests presenteeism costs more than absenteeism in knowledge-economy roles
- Attrition: talent loss to organisations perceived as psychologically unsafe; in competitive markets like India's IT and financial services sectors, this is among the most expensive costs an employer faces
For greater insights on How Poor Mental Health Impacts Workplace Productivity and Business, read our companion piece on Mental Health at Workplace in India: A Complete Guide for Employers & Employees (2026)
A BMC Public Health 2024 study on Indian workplaces found that India's hierarchical workplace structures significantly increase employee reluctance to disclose behavioral health concerns, making detection dependent almost entirely on manager capability and organisational culture rather than self-referral. Research found that 67% of employees with depression experienced workplace discrimination or adverse treatment during job applications. These are not soft HR concerns: they are organisational risk factors with measurable financial consequences.
💡Key Insight: The WHO-led evidence base shows that every USD 1 invested in mental health care returns USD 4 in economic and health gains. That return is not a projection. It is measured across multiple countries and multiple employer sizes. For Indian HR leaders making the business case to leadership, this ratio is the most credible single data point available.
Common Behavioral Health Conditions Seen in Indian Workplaces
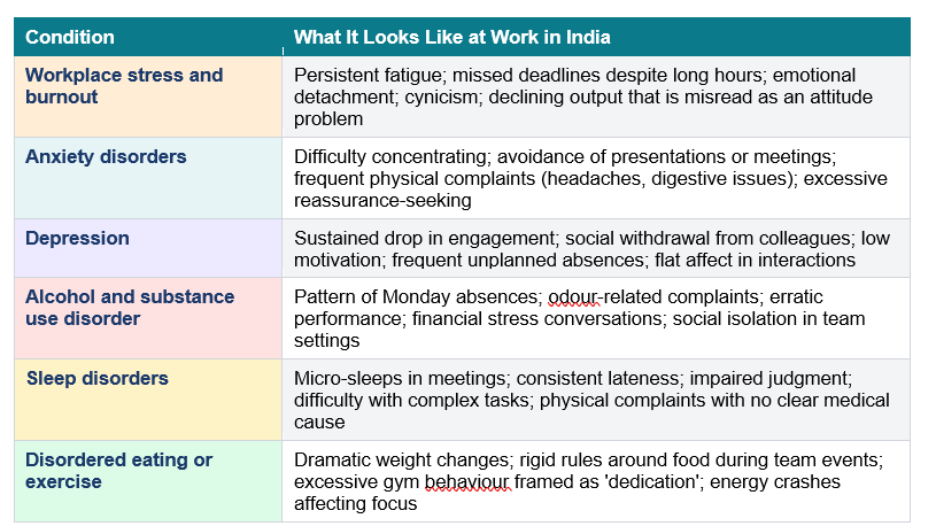
Behavioral health services are most needed when conditions are identified early. The table below maps the most common behavioral health conditions in Indian workplaces against how they actually present at the desk, in meetings, and in attendance patterns.

Workplace Stress Triggers Specific to India
- Extended working hours and the 'always-on' WhatsApp and Teams culture that has normalised after-hours availability
- Stringent deadlines combined with unclear or shifting project scope in project-delivery environments
- Micromanagement in hierarchical organisations where questioning upward is culturally discouraged
- Job insecurity following the 2023-24 tech layoff wave and ongoing gig economy precarity
- Financial pressure on first-generation earners who carry extended family financial obligations alongside personal EMIs
Behavioural health concerns in Indian workplaces are often identified late, largely due to stigma and hierarchical cultures that discourage early disclosure. As a result, issues may remain unaddressed for months before becoming visible.
Additional Risk Context in Indian Workplaces
Certain groups may face higher behavioral health risk due to structural and social pressures:
- LGBTQ+ employees: may experience identity-related stress, lack of workplace acceptance, or exclusion
- Gig and contract workers: face job insecurity, lack of benefits, and limited access to support systems
- First-generation corporate employees: often navigate financial pressure alongside workplace expectations
These factors can increase vulnerability and make access to confidential support systems even more critical.
Important to Note: Signs commonly misread as performance issues in Indian workplaces: persistent fatigue, irritability, difficulty concentrating, recurring physical complaints (headaches, back pain, digestive problems), social withdrawal, and sudden drops in engagement. Before a performance management process is initiated, the question every manager and HR professional should ask is: Could this be a behavioral health issue? The answer changes the intervention completely.
When to Seek Professional Help at Work
Not every dip in performance is a concern. But support should be considered when patterns persist.
- Changes in behaviour or performance continue for 2–3 weeks or more
- Stress or low mood is affecting concentration, productivity, or interactions
- Fatigue, irritability, or withdrawal is noticeable and sustained
- Performance does not improve with feedback or workload adjustments
At this stage, early support can make a significant difference.
- Employees can access confidential counselling through EAP providers such as 1to1help
- Managers and HR leaders should approach with concern, not judgement, and encourage support early
Behavioral Health Services Available in India
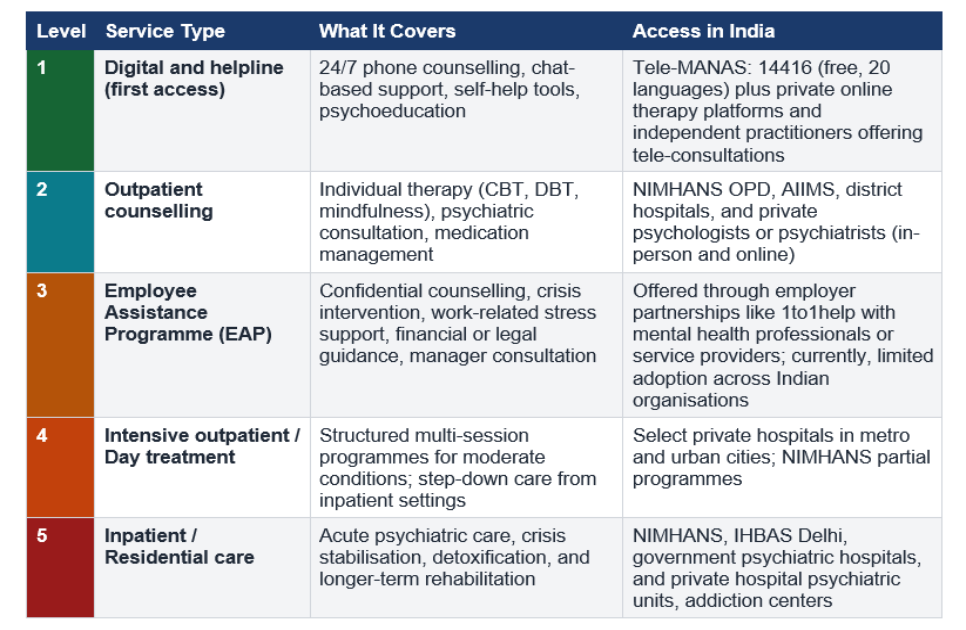
Behavioral health services in India span a spectrum from free government helplines to specialised inpatient care, with a growing mix of public systems and private practitioners improving access across regions.
Public and Private Behavioral Health Infrastructure in India
- Public sector backbone: NIMHANS, AIIMS, and the District Mental Health Programme (DMHP) provide structured, subsidised care across 767+ districts.
- Tele and crisis access: Tele-MANAS ensures free, multilingual, 24/7 support.
- Private care expansion: Independent psychologists, psychiatrists, and clinics deliver both in-person and digital services, significantly improving accessibility and reducing wait times.
- Policy framework: The National Mental Health Programme anchors service delivery and scale-up across the country.
What Is an Employee Assistance Programme (EAP) and How Does It Work?
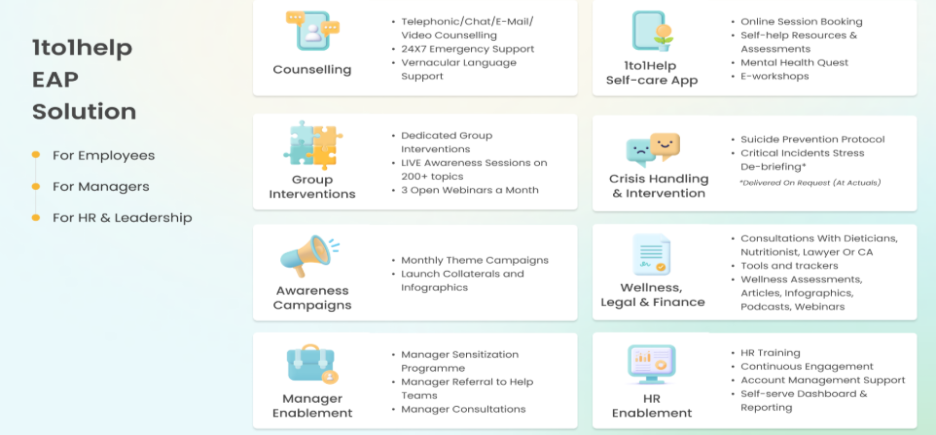
An Employee Assistance Programme (EAP) is a confidential, employer-funded support system that provides employees and their immediate families with access to psychological counselling, stress and burnout support, financial and legal guidance, and crisis intervention. It is the primary organisational mechanism for employee behavioral health support in the corporate sector.
In India, EAPs typically offer 24/7 phone and digital access, video counselling, multilingual support (critical for non-metro and manufacturing workforces), and manager coaching. It additionally provides access to crisis care, workshops, and digital self-care tools, enabling employees to seek help early and maintain emotional balance at work and beyond.
A defining feature is confidentiality: employers do not know which employees access EAP services unless the employee provides explicit written consent. EAP use is not included in performance records or appraisals, which helps ensure employees can seek support without fear of workplace consequences. This privacy protection is the single most important factor in driving uptake.
The gap between availability and adoption is significant. Only an estimated 0.1% of India's 1.1 million registered companies have implemented structured EAPs, and utilisation rates remain at just 5-10% even where programmes exist, primarily due to stigma and lack of awareness. Treatment gap context: 70-92% of people with mental disorders in India receive no treatment at all; India has 0.75 psychiatrists per 100,000 population against a WHO recommendation of 3.
💡Pro-Tip: If your organisation is implementing an EAP for the first time, do not launch with a company-wide email and a helpline number. Launch with a manager briefing first. Research consistently shows that employees access EAPs most frequently when a trusted manager makes a warm, normalising referral. Manager buy-in is the single most cost-effective driver of EAP utilisation.
How Indian Organisations Can Build a Behavioral Health-Supportive Workplace
Building a genuinely behavioral health-supportive workplace in India requires interventions across multiple layers. Focusing on isolated initiatives like workshops or helplines creates visibility, but not sustained impact. Organisations need coordinated action across policy, systems, managers, employees, and external ecosystems.
1. Policy Level: Create a Formal Foundation
At the policy level, organisations should:
- Develop and implement a Workplace Behavioral Health Policy that clearly defines scope, confidentiality, and escalation pathways
- Align internal policies with the Mental Healthcare Act to ensure employee rights and non-discrimination
- Integrate behavioral health into CSR initiatives under the Companies Act, particularly under employee well-being and community mental health
- Include behavioral health within ESG and well-being reporting frameworks
2. Organisational Level: Build Systems and Access
At the organisational level, the focus should be on infrastructure and access:
- Implement a structured Employee Assistance Programme (EAP) that includes:
- Confidential EAP counselling (short-term therapy support)
- Crisis intervention services
- Work-life and stress management support
- Conduct annual psychosocial risk assessments to identify burnout, workload imbalance, and toxic work patterns
- Train HR teams to identify early behavioral health concerns and respond appropriately
- Establish clear referral pathways to internal and external mental health professionals
- Build a psychologically safe culture where seeking help is normalised
3. Managerial Level: Strengthen Frontline Support
Managers are often the first point of contact, making this level critical:
- Train managers in empathy, active listening, and supportive communication
- Conduct regular structured one-on-one check-ins focused on well-being, not just performance
- Use anonymous pulse surveys to monitor team stress and morale
- Create clear protocols for referring employees to EAP counselling services without stigma or breach of confidentiality
- Equip managers to recognise early warning signs such as withdrawal, irritability, or performance decline
4. Employee Level: Enable Self and Peer Support
At the employee level, organisations should build awareness and coping capacity:
- Offer Cognitive Behavioural Therapy (CBT-based) and mindfulness workshops for stress and anxiety management
- Provide yoga, resilience, and emotional regulation programmes tailored to Indian contexts
- Create peer support networks or buddy systems within teams. 1to1help’s Emotional Care Champions programme is a very good example for the same.
- Train employees in mental health first aid to support colleagues safely
- Include financial wellbeing sessions, recognising the link between financial stress and mental health
5. Community Level: Extend the Support Ecosystem
No workplace operates in isolation; external linkages are essential:
- Build referral partnerships with institutions such as National Institute of Mental Health and Neurosciences for specialised care
- Collaborate with credible helplines and community-based mental health services for escalation support
- In addition to EAP counselling, integrate Tele-MANAS (14416) as a no-cost, 24/7 first-access resource for employees and their families
- Provide employees with clear guidance on when and how to seek external help
The Role of HR in Employee Behavioral Health Support
HR's role in employee behavioral health is to serve as the bridge between leadership commitment and employee access to support. This is neither a clinical role nor a counselling one. It is about building the right support systems within the organisation: HR designs the structures, removes the friction, and creates the conditions in which employees can access support safely.
Practical HR actions with demonstrable impact include: running regular destigmatisation campaigns that feature real employee stories with consent; integrating behavioral health into onboarding as a standard rather than an afterthought; building confidential reporting channels that do not route through line management; and conducting annual behavioral health audits using anonymous survey data.
Manager training makes support much more effective. The BMC Public Health 2024 India study found that when managers respond to disclosed distress with empathy rather than discipline, employees are three times more likely to seek help early. This is the highest-ROI single intervention available to HR. In Indian workplaces, hierarchy can limit open conversations, making psychological safety something that must be built intentionally.
💡Key Insight: India's workplace culture includes a strong norm of 'professional stoicism': employees are expected to separate personal problems from professional performance. This norm is not inherently wrong, but it becomes dangerous when it prevents disclosure of genuine behavioral health challenges. HR teams that name this norm explicitly, and offer structured, confidential alternatives to it, consistently see higher EAP uptake than those that simply make support available without addressing the cultural barrier.
Behavioral Health Best Practices for Indian Employers
The following best practices draw on the Indian Psychiatric Society model, Frontiers in Public Health research on Indian workplace interventions, and documented outcomes from large Indian corporate programmes.
1. Normalise the Conversation
- Discuss behavioral health as openly as physical health through internal campaigns
- Use leadership-led communication, storytelling, and visible endorsement
- Leverage days like World Mental Health Day for structured programming
Case: A large IT firm introduced quarterly well-being town halls in which senior leaders shared personal experiences of burnout.
Impact: Counselling uptake increased, reflecting higher trust and reduced stigma.
2. Make Support Accessible and Confidential
- Ensure 24/7 access to support via phone or digital platforms
- Provide multilingual counselling including Hindi and regional languages
- Clearly communicate confidentiality policies during onboarding and reinforce annually
- Offer structured EAP counselling services with defined privacy safeguards
Case: A manufacturing company enabled multilingual tele-counselling for plant workers across locations.
Impact: Usage increased among employees who had previously avoided seeking help.
3. Train the Ecosystem, Not Just Employees
- Train managers in empathy, active listening, and early identification
- Build HR capability for handling behavioral health concerns sensitively
- Conduct leadership orientation programmes to align tone from the top
- Move beyond one-off employee workshops to systemic capability building
Case: A BFSI organisation shifted from employee webinars to mandatory manager training on early identification and referral.
Impact: Earlier interventions reduced escalation to crisis-level situations.
4. Use Data, Not Stigma
- Conduct anonymous annual behavioral health surveys
- Track indicators such as stress, sleep, burnout, and engagement
- Use aggregated insights to design interventions without exposing individuals
- Build a business case for mental health using data trends
Case: A startup used anonymous surveys to identify high stress and sleep issues among employees.
Impact: Workload restructuring and flexible hours improved retention and productivity.
5. Integrate Behavioral Health into Performance Frameworks
- Move beyond the binary of “performance issue” versus “medical leave”
- Create graduated support pathways for employees showing early signs of distress
- Encourage early disclosure without fear of negative evaluation
- Document these pathways clearly in HR policies
Case: A consulting firm introduced a performance support pathway allowing temporary workload adjustments with counselling access.
Impact: Attrition among high-performing employees reduced significantly.
6. Build Community Partnerships
- Establish referral pathways with public institutions such as NIMHANS and private institutions/clinics
- In addition to EAP counselling helpline, consider integrating Tele-MANAS (14416) as a free, 24/7 support option
- Provide employees with clear escalation routes for crisis situations
- Use public infrastructure to extend care beyond what the organisation can internally provide
Case: A logistics company integrated Tele-MANAS into employee communication for its distributed workforce.
Impact: Access to immediate support improved, especially in remote locations.

💡Key Insight: In the Indian context, behavioral health strategy succeeds when it is normalised, accessible, systemically supported, data-driven, and externally connected. Organisations that operationalise these principles move beyond awareness into measurable impact.
💡Pro-tip: One of the highest-impact, lowest-cost behavioral health interventions available to any Indian employer is mandating that managers use the phrase 'How are you doing?' in at least one 1:1 per month, with training on what to do when the answer is not 'fine'. This is not therapy. It is early detection, and it works.
Behavioral Health and India’s Legal and Policy Framework
Indian employers have both explicit and implicit legal obligations related to behavioral health. Understanding this framework is important not only for compliance but for using existing legislation as leverage when building internal behavioral health programmes.
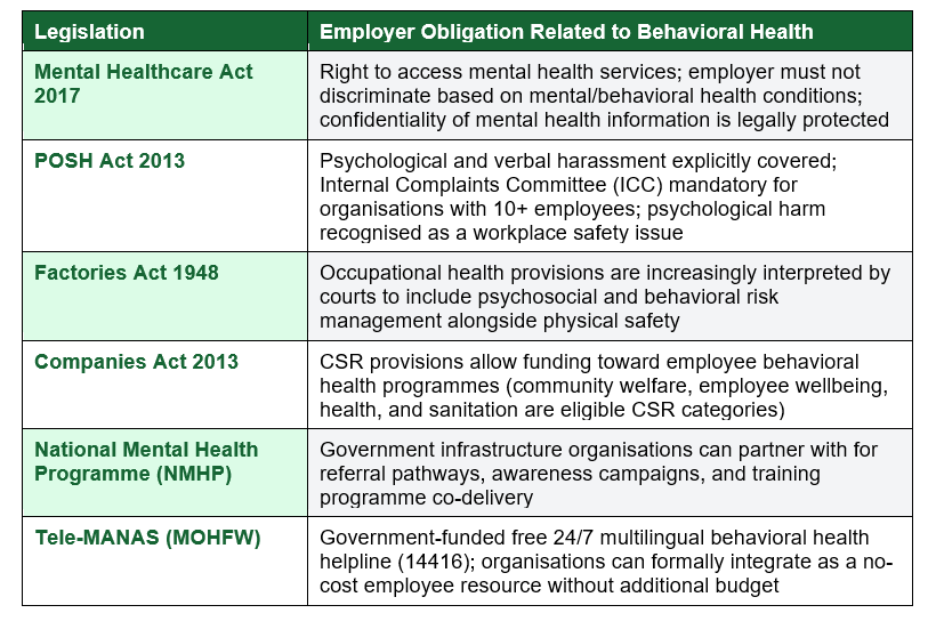
Legal Note: The Mental Healthcare Act 2017 is the most significant piece of legislation affecting workplace behavioral health in India. It establishes the right to access mental health services, protects confidentiality, and prohibits employment discrimination based on mental or behavioral health conditions. If your organisation does not have a formal non-discrimination clause in its HR policy that references the MHCA 2017, add one. It signals legal literacy and reduces liability.
Conclusion
Riya, the project manager from our opening, is a composite of real patterns playing out across hundreds of thousands of Indian workplaces right now. She is not unusual. She is not dramatic. She is simply unsupported in a way that her employer has the means, and increasingly the legal obligation, to change.
Behavioral health in the Indian workplace is not just a Western concept or an HR aspiration. It is a practical, evidence-backed framework for addressing the actual conditions that are reducing productivity, driving attrition, and costing Indian organisations billions of rupees annually. The organisations that treat it as such will have a demonstrable advantage in both performance and talent retention in the decade ahead.
With the right support in place, employees can stabilise, recover, and continue to perform effectively.
If your organisation is ready to take action, start with an honest audit of what you currently offer. Speak to your employees anonymously to understand what they actually need. At the same time, organisations should move beyond awareness and put structured support in place. Partnering with a professional EAP provider such as 1to1help can enable confidential counselling, early intervention, and sustained employee support at scale.
The shift is straightforward but non-negotiable: from reactive support to proactive behavioral health systems. Organisations that act now will not only protect their people but also build more resilient, productive, and future-ready workplaces.
FAQs
Q1. What is behavioral health in simple terms?
Behavioral health refers to how your daily habits, behaviours, and emotional responses affect your overall mental and physical wellbeing. It covers sleep patterns, substance use, stress management, eating habits, and how you cope with life's challenges. In the Indian context, behavioral health is an emerging term describing a more holistic approach: recognising that your actions are deeply connected to your mental and physical health. While often used alongside 'mental health', behavioral health specifically emphasises the role of behaviour in shaping wellness, making it particularly relevant for workplace wellness programmes and preventive healthcare.
Q2. Is behavioral health the same as mental health in India?
Not exactly. Mental health is a subset of behavioral health. Mental health focuses on your emotional, psychological, and cognitive state: how you think, feel, and relate to others. Behavioral health is a broader concept that includes mental health but also addresses how behaviours such as sleep, diet, physical activity, and substance use affect your total wellbeing. In India, both terms are often used interchangeably in healthcare and corporate settings, but distinguishing them helps organisations design more comprehensive wellness programmes that address both psychological conditions and the behavioral patterns that reinforce them.
Q3. What behavioral health services are available for employees in India?
Indian employees can access a growing range of behavioral health services across public systems, workplaces, and private care providers. Government offerings include Tele-MANAS (14416), which provides free, 24/7 support in 20 languages, the District Mental Health Programme, and specialised care through institutions such as NIMHANS and AIIMS. In the corporate sector, Employee Assistance Programmes (EAPs) offer confidential counselling, crisis intervention, and support for work-related, financial, and personal concerns. Alongside this, private psychologists and psychiatrists provide in-person and online therapy, with digital consultations increasingly improving access and convenience.
Despite this expanding ecosystem, structured EAP adoption in India remains limited, and access remains uneven. Employees in urban areas typically have significantly better access to behavioral health services compared to those in semi-urban and rural settings.
Q4. How do I know if an employee may have a behavioral health issue?
Behavioral health challenges at work rarely look like textbook diagnoses. Common signals include a noticeable drop in productivity or engagement, persistent fatigue, increased irritability or emotional withdrawal, frequent physical complaints, difficulty concentrating, and higher-than-usual absenteeism. In India, these signs are frequently misread as performance problems or dismissed due to stigma. Managers trained in behavioral health awareness are better equipped to distinguish distress from disengagement and respond with empathy rather than discipline. Creating psychologically safe environments where employees feel comfortable speaking up is the most effective long-term detection strategy.
Q5. What is an EAP and how does it help with behavioral health?
An Employee Assistance Programme (EAP) is a confidential, employer-funded support system that helps employees manage personal and professional challenges affecting their wellbeing and work performance. EAPs cover psychological counselling, stress and burnout support, crisis intervention, financial guidance, legal assistance, and work-life balance resources. In the context of behavioral health, EAPs serve as the structured first line of support: employees access professional help without fear of disclosure to their employer. In India, EAP utilisation remains at an estimated 5-10%, partly due to stigma and lack of awareness, but organisations investing in EAPs report improved retention, lower absenteeism, and measurably stronger productivity outcomes.
Q6. Is behavioral health treatment confidential in India?
Yes. India's Mental Healthcare Act 2017 mandates confidentiality: healthcare providers and employers are legally required to protect an individual's mental health information. Employee Assistance Programmes operate under strict confidentiality protocols; employers do not receive information on which employees access EAP services unless the employee provides explicit written consent. This protection is critical in the Indian context, where stigma remains a primary barrier to help-seeking. Employees should be clearly informed of these confidentiality rights during onboarding and through regular HR communications.
Q7. What are the legal obligations of Indian employers regarding behavioral health?
Indian employers have both explicit and implied legal obligations. The Mental Healthcare Act 2017 prohibits employment discrimination based on mental or behavioral health conditions. The POSH Act 2013 requires organisations with 10+ employees to establish an ICC to address psychological and verbal harassment. The Factories Act 1948 includes occupational health provisions increasingly interpreted to cover psychosocial risks. The Companies Act 2013 allows CSR funding to be directed toward behavioral health programmes. Cumulatively, these frameworks make proactive behavioral health support not only ethical but a compliance priority for any organised Indian employer.
Related Articles That You Will Find Helpful
References
- American Medical Association. (n.d.). What is behavioral health? https://www.ama-assn.org/public-health/behavioral-health/what-behavioral-health
- American Psychiatric Association. (n.d.). Diagnostic and statistical manual of mental disorders (DSM–5). https://www.psychiatry.org/psychiatrists/practice/dsm
- APAC Entrepreneur. (n.d.). How to support first-generation professionals in the workplace. https://apacentrepreneur.com/how-to-support-first-generation-professionals-in-the-workplace/
- Cleveland Clinic. (n.d.). Cognitive behavioral therapy (CBT). https://my.clevelandclinic.org/health/treatments/21208-cognitive-behavioral-therapy-cbt
- Cleveland Clinic. (n.d.). Depression. https://my.clevelandclinic.org/health/diseases/9290-depression
- Cleveland Clinic. (n.d.). Substance use disorder. https://my.clevelandclinic.org/health/diseases/16652-drug-addiction-substance-use-disorder-sud
- Devdoot. (n.d.). Why mental health at work in India is failing. https://devdoot.org/blogs/leadership-culture/mental-health-work-india-eap-failing
- Economic Times HR. (2024). Why mental health still remains in shadows. https://hr.economictimes.indiatimes.com/news/workplace-4-0/employee-wellbeing/why-mental-health-still-remains-in-shadows/129687770
- Frontiers in Public Health. (2022). Workplace mental health and well-being. https://www.frontiersin.org/journals/public-health/articles/10.3389/fpubh.2022.800880/full
- Government of India. (1948). The Factories Act, 1948. https://www.indiacode.nic.in/bitstream/123456789/15097/1/factory_acta1948-63.pdf
- Government of India. (2013). The Companies Act, 2013. https://www.indiacode.nic.in/bitstream/123456789/2114/5/A2013-18.pdf
- Government of India. (2017). The Mental Healthcare Act, 2017. https://www.indiacode.nic.in/bitstream/123456789/2249/1/A2017-10.pdf
- Healthline. (n.d.). What is behavioral health? https://www.healthline.com/health/mental-health/what-is-behavioral-health
- IBM. (n.d.). Environmental, social, and governance (ESG). https://www.ibm.com/think/topics/environmental-social-and-governance
- Indian Journal of Psychiatry. (2024). Mental health and well-being at the workplace. https://journals.lww.com/indianjpsychiatry/fulltext/2024/66002/mental_health_and_well_being_at_the_workplace.16.aspx
- Investopedia. (n.d.). Presenteeism. https://www.investopedia.com/terms/p/presenteeism.asp
- Ministry of Health and Family Welfare. (2022). Tele-MANAS: National Tele Mental Health Programme. https://telemanas.mohfw.gov.in/home
- Ministry of Health and Family Welfare. (n.d.). District Mental Health Programme. https://nhm.gov.in/index1.php?lang=1&level=2&sublinkid=1043&lid=359
- Ministry of Information and Broadcasting. (2024). Government initiatives for mental health. https://www.pib.gov.in/PressReleasePage.aspx?PRID=2100706®=3&lang=2
- Mindful. (n.d.). Getting started with mindfulness. https://www.mindful.org/meditation/mindfulness-getting-started/
- MyndStories. (2026). India Budget 2026 prioritizes mental health. https://myndstories.com/news/india-budget-2026-prioritizes-mental-health
- Owens, B., Mills, S., Lewis, N., & Guta, A. (2022). Work-related stressors and mental health among LGBTQ workers: Results from a cross-sectional survey. PLOS ONE, 17(10), e0275771. https://doi.org/10.1371/journal.pone.0275771
- Positive Psychology. (n.d.). Maladaptive coping. https://positivepsychology.com/maladaptive-coping/
- PubMed. (2024). Mental health workplace study. https://pubmed.ncbi.nlm.nih.gov/39004708/
- PubMed Central. (2022). Mental health prevalence and workplace implications. https://pmc.ncbi.nlm.nih.gov/articles/PMC9110774/
- PubMed Central. (2024). Behavioral health systems research. https://pmc.ncbi.nlm.nih.gov/articles/PMC11247900/
- Qualtrics. (n.d.). Employee pulse surveys. https://www.qualtrics.com/articles/employee-experience/what-is-employee-pulse-survey/
- Verywell Mind. (n.d.). Active listening. https://www.verywellmind.com/what-is-active-listening-3024343
- Verywell Mind. (n.d.). Empathy. https://www.verywellmind.com/what-is-empathy-2795562
- World Health Organization. (n.d.). International classification of diseases (ICD). https://www.who.int/standards/classifications/classification-of-diseases
- World Health Organization. (2024). Mental health at work. https://www.who.int/news-room/fact-sheets/detail/mental-health-at-work
- World Health Organization. (2025). Over a billion people living with mental health conditions. https://www.who.int/news/item/02-09-2025-over-a-billion-people-living-with-mental-health-conditions-services-require-urgent-scale-up
- Zenodo. (n.d.). A study on factors affecting stress levels among gig economy workers. https://zenodo.org/records/19518040





.png)